Traumatic Brain Injury
Traumatic brain injury leaves millions of survivors with substantial impairments in physical, emotional, cognitive, and behavioral consequences each year. Despite high-tech diagnostic and treatment protocols, mainstream medicine has managed to do little to overcome these long-term pathologies. The recent discovery that traumatic brain injury, by damaging the brain’s hypothalamus, triggers dysfunction of the pituitary gland, we identify and treat the resulting hormonal deficiencies in patients with traumatic brain injury. Restoring hormone levels to their optimal, pre-injury and youthful levels results in remarkable recovery of many of the impaired functions.
Traumatic Brain Injury Hormone Treatment
Restoring the balance of deficient hormones to their pre-injury levels has been shown to produce substantial improvements in all facets of traumatic brain injury.
Despite powerful evidence for hormone replacement, conventional physicians remain unwilling to provide this vital therapy.
Salus Clinic treats brain-injured patients, balancing their deficient hormones and achieving remarkable recovery, even in patients who are years out from their original injury.
If you have had a traumatic brain injury, schedule your initial evaluation today.
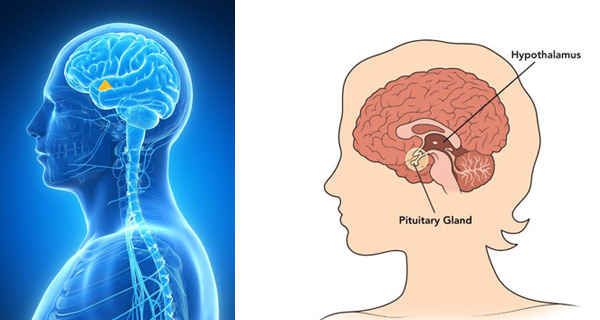
Most people typically think of hormones as the products of the endocrine glands located throughout the body. That’s an accurate, but incomplete, view of these powerful biological regulatory molecules. Virtually all endocrine glands are under the control of the pituitary gland, which is located inside the skull at the base of the brain. Because of its powerful influence on the other endocrine glands, the pituitary is often referred to as the “master gland.”
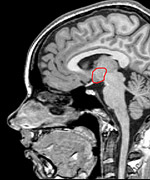 |
The area circled in red is the hypothalamus – the control center for the pituitary gland and production of hormones throughout the body. |
But even the pituitary is subject to a “higher” form of control. An ancient brain structure called the hypothalamus has a direct connection to the pituitary via a unique network of veins. Regulatory molecules from the hypothalamus “tell” the pituitary how much of its own hormones and hormone releasing factors to produce. And the hypothalamus, as part of the brain itself, receives constant neurological inputs from all over the body, creating a host of feedback loops. It is those feedback loops that maintain a steady balance between extreme biochemical states.
That connection between the brain’s hypothalamus and the endocrine system’s pituitary is called neuroendocrine function. And, though it may seem obvious, medical science is only just beginning to recognize that trauma to the brain, even apparently minor trauma, can damage the hypothalamic-pituitary system and have profound effects on hormonal function.
In fact, most people (including the majority of physicians) assume that the neurological deficits that follow a traumatic brain injury result simply from disruption to brain tissue itself. In this simplistic model, a “hit” to the head causes the brain to be “rattled,” triggering bleeding, bruising, and other large-scale injuries that can be seen on MRI and CT scans. And it’s quite true that we can predict some of the deficits a brain-injured person will sustain by the location and severity of the visible damage on those scans.
But victims of traumatic brain injury frequently have sustained neurological deficits that exceed what would be predicted simply by examining brain scans. Unfortunately, people with so-called minor traumatic brain injury, who comprise the largest group of brain-injured patients, have no visible damage at all on brain scans.
It took someone with genuine insight and a fresh approach to recognize that it is disrupted hormonal function, not simply physical “brain damage,” that creates the sustained neurological deficits suffered by victims of traumatic brain injury.

